New mechanism discovered for cognitive disorders in schizophrenia

- Schizophrenia mechanism: Scientists have discovered that oligodendrocytes play a key role in the cognitive disorders of schizophrenia. The genetic risk affects not only neurons but also these cells.
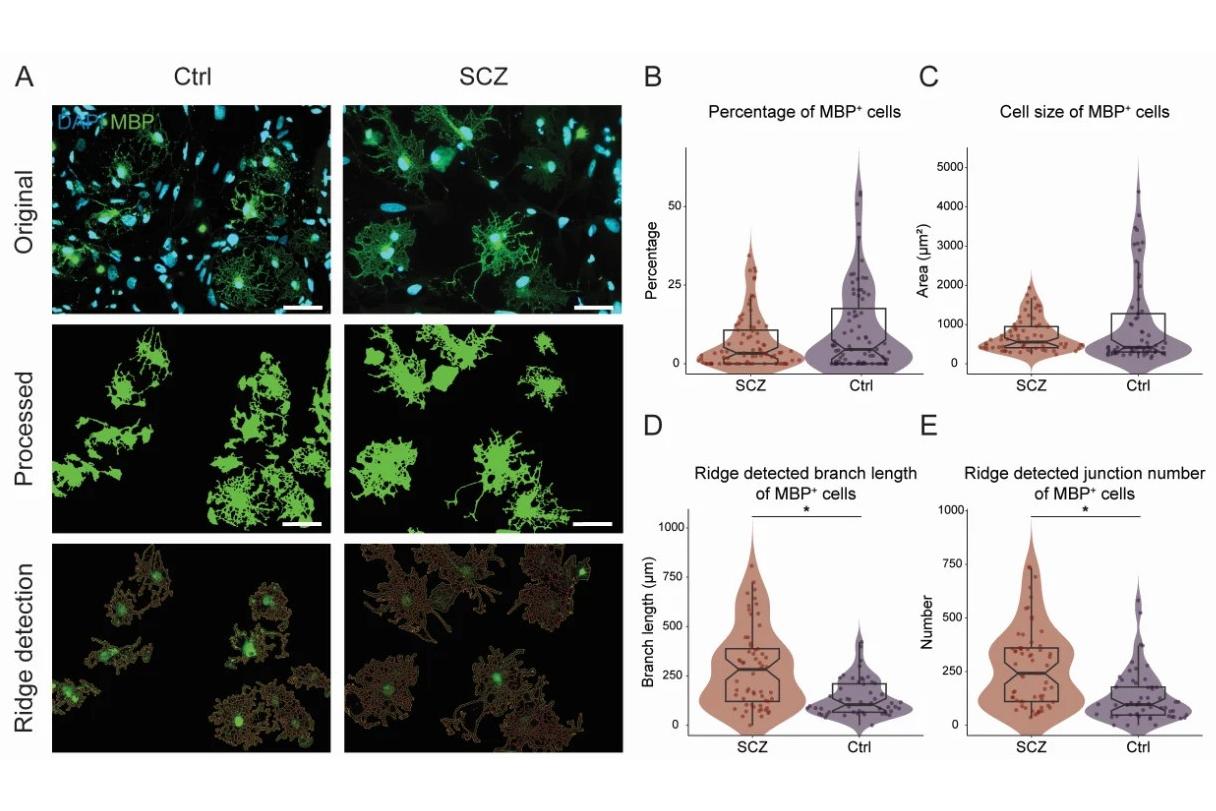
- Morphology: Surprisingly, oligodendrocytes from schizophrenia patients showed a more complex morphology and were more mature in cell culture than those from healthy controls. This discovery could indicate a special developmental status of the cells.
- Personalized medicine: Research findings could potentially lead to better stratification of schizophrenia patients for personalized therapies.
Schizophrenia is a serious psychiatric disorder that affects around one percent of the population worldwide and is notoriously difficult to treat. The medications currently available for schizophrenia can alleviate so-called positive symptoms such as hallucinations and delusions. However, there is still a huge need to treat the so-called negative symptoms such as social withdrawal and lack of motivation, as well as cognitive symptoms such as attention and memory disorders.
Peter Falkai, Director of the Department of Psychiatry and Psychotherapy at the LMU Klinikum and Director of the Research Clinic of the Max Planck Institute of Psychiatry (MPI) and his team led by former International Max Planck Research School for Translational Psychiatry (IMPRS-TP) PhD student Florian Raabe have developed a fast and robust protocol for oligodendrocytes derived from induced pluripotent stem cells (iPSC). Oligodendrocytes are cells in the nervous system that produce myelin; this layer insulates the axon that connects nerve cells. This insulation enables faster signal transmission from neuron to neuron. The team took blood samples from the so-called white matter of schizophrenia patients with clinical impairments to generate iPSCs that differentiated into oligodendrocytes in cell culture. Schizophrenia patients appear to have extensive white matter disorders.
The team hypothesized that this feature may indicate a "pre-maturation" phenotype in the early developmental stage of oligodendrocytes. The protocol used in this study allowed the researchers to examine only the early developmental stages, which are distinctly different from the late developmental stages of oligodendrocytes as observed in postmortem studies.
"The current study is only a preliminary investigation, there are still many experiments we would like to conduct. Firstly, we would need to increase the sample size to see if the results are transferable to a larger cohort. Secondly, we would like to know more about the function of these oligodendrocytes in schizophrenia: whether their ability to myelinize is also impaired and how they interact with other cells," explains Raabe. He is now a senior physician at the MPI Research Clinic and will continue his work there by cultivating the oligodendrocytes with iPSC-derived neurons or even creating three-dimensional spheroids or organoids to recreate the environment of the human brain.
Looking back, Falkai can now summarize many years of successful research: "In the first postmortem study 13 years ago, I thought that the interneurons must be involved. I would never have dreamed that there would also be a circumscribed reduction in oligodendrocytes. Although we still cannot answer the question of whether the pathology of oligodendrocytes in schizophrenia is primary or secondary with certainty, we believe that oligodendrocytes definitely play a central role in the pathogenesis of schizophrenia and serve as a new starting point for the development of better therapies. The very first mechanism for cognitive dysfunction in schizophrenia that we have found should hopefully be further investigated in the coming years. We also believe that schizophrenia is a heterogeneous disorder. We have only studied samples from schizophrenia patients with white matter deficits: If these phenotypes are specific to a certain group of patients, this could mean possible stratification of patients for personalized medicine in the future."
Publication
iPSC-modeling reveals genetic associations and morphological alterations of oligodendrocytes in schizophrenia
Man-Hsin Chang, Jan Benedikt Waldeck, Marius Stephan, Nirmal Kannaiyan, Valéria de Almeida, Emanuel Boudriot, Temmuz Karali, Lukas Röll, Laura Fischer, Damianos Demetriou, Nadia Gabellini, Sabrina Galinski, Andrea Schmitt, Sergi Papiol, Daniel Keeser, Peter Falkai, Moritz J. Rossner and Florian J. Raabe
Translational Psychiatry, 2025
contact
Prof. Dr. Peter Falkai
Director of the Department of Psychiatry and Psychotherapy at LMU Klinikum München

